Translated from the ancient Greek language, osteochondrosis means ὀστέον - bone and χόνδρος - cartilage, and is characterized by complex degenerative changes in the articular elements of the bone skeleton. Almost every part of the skeletal framework is susceptible to this neurological disease. Thoracic and / or cervical vertebral discs may be in the affected area. However, it is osteochondrosis of the lumbar spine, the symptoms and treatment of which are the most common in modern conditions, which is the reason for the discussion and concern of practicing neuropathologists.
Pathogenesis, or development of the inflammatory process
Every organism in the process of growth changes its physiology. So because of this, diffuse changes occur in the vascular bed of the skeletal intervertebral discs. The supply of nutrients to the lumbar spine is complicated by various traumatic conditions and / or constant dynamic loads in this part of the spinal cord. Insufficiency in nutrition with the necessary microelements is further complicated by osteochondrotic processes leading to loss of elastic characteristics and strength of cartilage joints. With lumbar spine osteochondrosis, the symptoms of the disease are most active with asymmetric and irrational work of the spinal muscles, which are detected in different conditions:
- insufficient heating of muscle tissue;
- wrong attitude;
- overload of intervertebral joints due to excess adipose tissue;
- use of mattresses on a soft base during a night’s rest;
- sharp mechanical and / or dynamic loads on the lumbar spine;
- physical stress;
- with exacerbation of chronic pathologies.
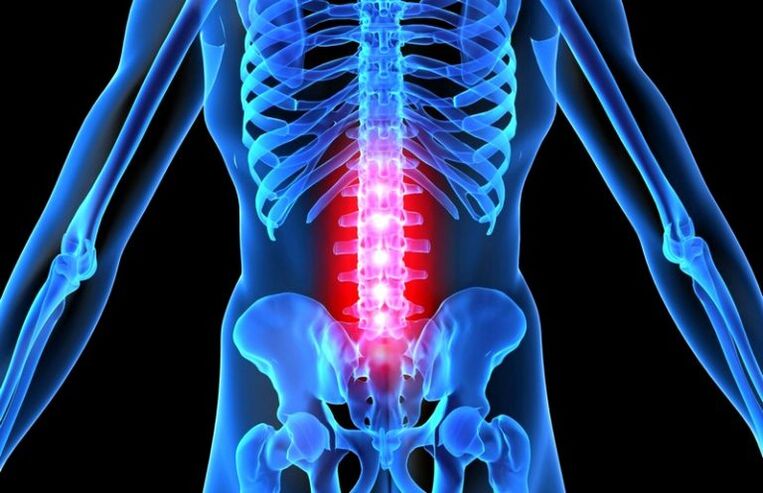
The supply of nutrients to the lumbar spine is complicated by various traumatic conditions and / or constant dynamic loads in this part of the spinal cord.
If lumbar osteochondrosis is detected, the symptoms of a neurological disease due to premature medical intervention can lead to more serious neurological pathologies, for example, sciatica, spinal hernia, intervertebral disc damage, and other complications.
Why does lumbar osteochondrosis occur?
To date, the problem of diffuse transformations in the intervertebral space has not been fully studied. With lumbar spine osteochondrosis, the symptoms of manifestations of neurological pathology are often felt by middle-aged people from 35 to 45 years.

Nervous overload, stressful situations can also lead to the onset of the disease.
Lupus at this most efficient age that static and dynamic stress occurs in the spine. However, according to expert observations, back pain is starting to bother more and more people of the younger age group. So already in the period from 18 to 25 years, young people become patients of neurological treatment departments. This is due to poor physical activity, excess weight, poor posture and general deformity of the joints, which cause lumbar osteochondrosis.
Symptoms and treatment of neurological pathology, it is desirable to identify and adequately respond to it at the earliest stage of disease formation.
Other risk factors that lead to lumbar spine osteochondrosis include:
- hereditary forms;
- insufficient supply of cartilaginous vessels with micronutrients;
- violation of metabolic processes due to various circumstances;
- uneven development of the musculoskeletal structure;
- sedentary lifestyle;
- disorders of the body associated with the work of the endocrine system;
- weakening of muscle structures due to the harmful effects of alcohol, smoking and other bad habits;
- consequence of various chronic pathologies;
- segmental instability of the spine elements;
- nervous overload, stressful situations and other constituents.
However, when you diagnose lumbosacral osteochondrosis, the symptoms of neurological pathology in women can be diagnosed due to disorganization or the development of disorders related to hormonal changes. At the age of 35 to 45 years, the female body begins to undergo significant physiological transformations, which affects the functional work of all areas of bone and cartilage of the spine.
Symptomatic signs of the disease
With osteochondrosis of the lumbosacral region, the symptoms of neurological pathology become felt with severe pain in the lumbar region, leading to numbness, discomfort, and a feeling of pain in the lower back. Lack of adequate appropriate therapy can complicate the situation and lead to complete atrophy of the muscle structures in the lumbosacral spine. An increase in pain can be provoked by various factors, for example, sneezing, coughing, sharp turns, and lifting heavy objects. Incisions occurring in the lumbar region are most often given to the gluteal region and the calf region of the lower limbs. With lumbosacral osteochondrosis, the symptoms of a neurological disease can be defined by the following signs:
- release of acute excruciating pain in the sacral region of the spine and in the organs in the pelvic region;
- loss of sensitivity;
- discomfort in the innervated lumbar spine muscles;
- hypotension and hypotrophy.

All of these symptomatic signs arise from damage to the nerve roots in the intervertebral discs of the lumbar spine.
Stages of the disease
When you diagnose lumbosacral osteochondrosis, the symptoms and treatment of the disease depend on the stage of the inflammatory process. So, according to the results of a diagnostic examination, it is possible to determine some specific signs of lumbar spine inflammation:
- The first stage is defined by mild sensations of pain in the lumbar area, which intensify under the influence of physical exertion. Only with sudden movements, the patient feels a sharp, aching or dull ache in the lower back. In a relaxed state, pain does not occur.
- The second stage is determined when the distance between the vertebral discs decreases, due to compression and the onset of degenerative-dystrophic formations in the annular fibrosus. A sharp pain radiating to the ankle region of the lower limbs, buttocks, and outside of the thigh is due to squeezing of the nerve endings between the discs in the vertebral space.
- Destruction of the annulus fibrosus occurs in the third stage of the disease, and this is the most favorable time for the formation of a hernia in the intervertebral disc. Severe pain in the lumbar region is permanent due to significant deformity in the lumbosacral spine.
- The last, fourth stage of lumbar spine osteochondrosis, the symptoms, treatment and rehabilitation of which are the most difficult in the whole process of destruction of the musculoskeletal system. This stage of the disease leads to the inability of the patient, as well as to his complete or partial immobility.
However, any form of osteochondrosis should not cause fear and panic in a person; only appropriate appropriate medical treatment is required.
Lumbar osteochondrosis: symptoms and medication
Based on the results of symptomatic signs and the establishment of an appropriate diagnosis according to the stage and form of the disease, specialists choose the appropriate treatment with medication, which is based on the use of pharmacological combinations of different orientations. The main objectives of the treatment in solving the problem are:
- slowing down degenerative-dystrophic processes in the lumbar area, through the implementation of appropriate therapeutic and prophylactic measures;
- elimination of functional disorders of the spinal nerve endings;
- neutralization of painful sensations;
- functional restoration of muscle tone of the lumbosacral region;
- return of the patient to active life.
The age and gender of the patient, as well as the condition of his endocrine system, play an important role in choosing a method of drug treatment.
The main emphasis in drug exposure is placed on pain elimination with proper selection of pharmacological analgesic agents. Anti-inflammatory drugs allow you to neutralize destructive processes in the muscular structures of the spinal region. The most effective pharmacological agents are non-steroidal anti-inflammatory groups.

The most effective pharmacological agents are non-steroidal anti-inflammatory groups.
With the ineffectiveness of NSAIDs (non-steroidal anti-inflammatory drugs), anesthetics with hormonal supplements and / or paravertebral blockade are used. Moreover, the complex drug process includes other types of pharmacological drugs, for example, sedatives, muscle relaxants, groups of drugs containing vitamins B1 and B12, which eliminate the effect of compression and ensure the supply of nerve tissue with micronutrients. After the end of the acute inflammatory period, treatment through drug therapy ends, and other therapeutic and prophylactic measures are used during the remission period.
Therapeutic prevention of lumbar osteochondrosis
You should be aware that the treatment of osteochondrosis is a complex process that requires strict discipline and strict adherence to all the recommendations of the attending physician. A prerequisite for complete recovery of the body is the performance of all phases of complex therapy, which includes:
- Massage that helps relieve muscle pain, restores blood circulation to problematic areas of the lumbar spine, eliminates muscle tension in these areas of the body.
- Physiotherapy is a great way to rehabilitate after an illness. Lack of side effects, elimination of residual stresses in the lumbar region, these are the advantages that physiotherapy procedures have.
- Manual therapy is capable of acting mechanically on the muscular tissues of the lower back to a measured extent and providing them with an improvement in all vital processes.

It should be remembered that non-compliance with the recommendations of the neuropathologist for the complex therapeutic treatment of lumbar osteochondrosis is a possible appointment with the surgeon. In 90% of cases, surgical intervention in the spinal sections is a consequence of a neglected condition of the disease and non-compliance with the recommendations of the attending physician.

























